Published on 11 May 2026
Precision medicine is reshaping nerve pain care by identifying the biological cause of nerve damage and guiding targeted, personalised treatment.
At a glance
-
Neuropathic pain affects hundreds of thousands of Singaporeans, yet many cases remain misclassified because conventional tests cannot pinpoint the cause of nerve damage.
-
Advanced diagnostics such as skin biopsy and molecular staining can reveal distinct drivers of nerve injury that standard imaging misses.
-
At NUH, biology-guided treatment of small fibre neuropathy has led to pain reduction and functional recovery, showing how personalised therapy can replace trial-and-error care.

Dr Amanda Chan explaining molecular staining findings to a patient.
Identifying the cause behind pain
Peripheral neuropathy is not a single disease but may be caused by a spectrum of biologically distinct conditions. In many patients, nerve damage is caused by metabolic stress, most commonly diabetes, which affects one in nine Singaporeans. In others, the immune system mistakenly targets peripheral nerve fibres — a mechanism that routine blood tests and imaging frequently fail to detect.
When the underlying cause remains hidden, pain is often labelled “idiopathic”, and treatment may be ineffective as the underlying cause cannot be managed in a targeted manner. Precision diagnostics aims to change this by uncovering the specific driver of nerve injury.
Dr Chan's lab focuses on identifying immune-mediated neuropathies, an under-recognised subgroup with distinct treatment implications. Using skin biopsy and molecular staining, her team can directly examine small nerve fibres at a cellular level. These thin fibres, which transmit pain and temperature signals, are too small to be detected by standard nerve conduction tests.
The biopsies can reveal early destruction and loss of nerve fibres, and immune activity surrounding blood vessels and nerves — changes that signal active disease and a higher risk of persistent pain.
"Early changes and loss of small nerve fibres and immune activation are strong warning signs,” Dr Chan said. “They tell us this is not just pain without a cause, but an ongoing biological process.”
Targeting treatment to the mechanism
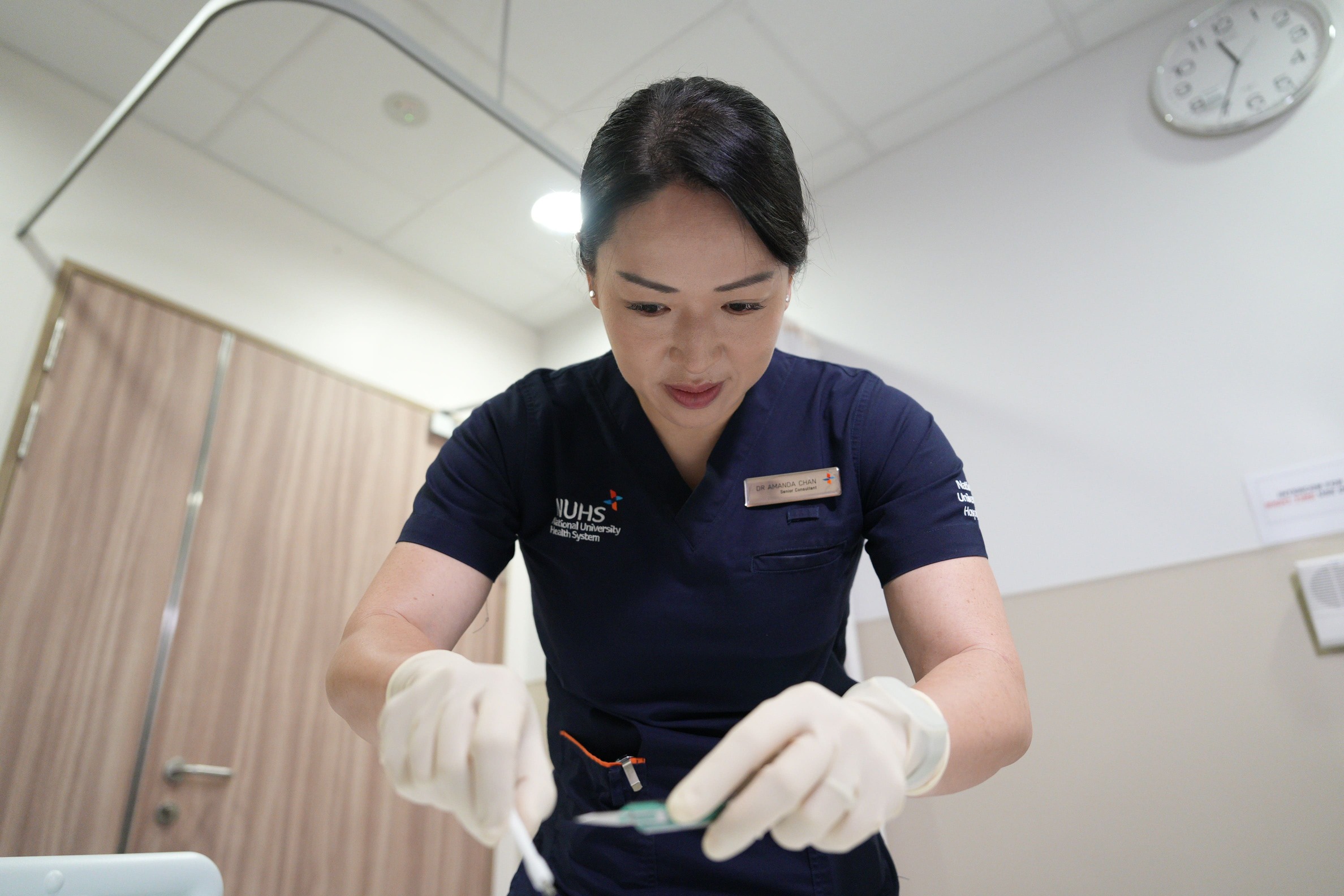
Dr Amanda Chan preparing for a skin biopsy procedure. Skin biopsy and molecular staining are central to identifying nerve fibre damage that standard tests cannot detect.
Once the mechanism is identified, treatment can be matched to the cause, a defining principle of personalised medicine.
“Using skin biopsy and molecular staining, we can directly visualise nerve fibre damage and immune activity that other tests cannot detect,” Dr Chan said.
A 2025 NUH study led by Dr Chan evaluated the efficacy of rituximab, an immunemodulating therapy, on five patients who had antibody-positive small fibre neuropathy that did not respond to conventional treatments. Instead of suppressing pain signals, the treatment targeted the immune process responsible for nerve injury.
The findings represent one of the first published case series globally to document rituximab's efficacy in antibody-positive small fibre neuropathy.
“For these patients, treatment shifted away from guesswork,” Dr Chan said.
“Immune-mediated pain was treated with immune therapy, while metabolic injury required metabolic control — aligning therapy with biology rather than symptoms alone.”
|
Key findings: 2025 NUH rituximab study Published in the Journal of Neuroimmunology, the study documented five cases of antibody-positive small fibre neuropathy treated with rituximab.
|
Reclassifying "unexplained" pains
One of the most significant effects of precision diagnostics has been the reclassification of patients previously labelled as having functional or unexplained pain.
"Lab findings have reclassified patients from 'unexplained pain' to confirmed neuropathy, avoiding ineffective treatments," Dr Chan said. "Patients gain validation, clearer explanations, and more focused care — with fewer repeat tests and referrals."
Where diagnosis once stretched across years and multiple specialists, a targeted diagnostic pathway can now be completed within months.
Implications for population health
At the population level, unresolved neuropathic pain gradually erodes mobility, independence and quality of life, particularly in an ageing society.
Reduced nerve fibre density and immune markers not only explain individual pain syndromes but also help identify patients who may benefit from early intervention.
Biology-guided care ensures patients receive right treatment from the outset, rather than cycling through medications with limited benefit. Dr Chan's team continues to develop biomarker panels that quantify immune and metabolic nerve injury, with the aim of integrating molecular diagnostics into routine clinical practice.
“When invisible nerve damage becomes visible, both doctors and patients finally have a clear path forward,” Dr Chan said.
In consultation with Dr Amanda Chan, Senior Consultant, Division of Neurology, Department of Medicine, NUH, and Assistant Professor, NUS Medicine.